How would the world and our lives change if we always healed without scars? Imagine a world where regardless of whatever we did or whatever happened to us there would be no consequences regarding scars. No scars, no signs of what had occurred..nothing! In this make-believe world surgeries would occur without scars. It would not matter what type of sutures were used, where the incisions were placed, genetics, or anything else. When all was said and done no trace of surgery would be present other than the final result of whatever change was desired.
Perhaps in the distant future, this will be the case. However, at the present moment, —even though we have made tremendous progress with our understanding of anatomy, physiology, healing, and surgery— there will be some form of scar, regardless of how thin and faint it may be. The goal of surgery, therefore, is how to control the things that we can control to reduce as much as possible the visibility of scars from any procedure.
Well, what are the factors that contribute to a better incision and scar? There are many but four broad categories are most important to discuss:
- Genetics
- The tension on the incision
- The amount and duration of inflammation
- Location and orientation of the incision
The first category, genetics, cannot be controlled (yet). The other three, therefore, are the ones that can and should be controlled to get the best scar appearance possible.
Tension on the incision: Our bodies have the ability to support some tension without healing poorly. The more tension an area experiences (think tummy tuck) the more stress on the tissue and its blood supply that occurs in the area. Blood supply is good, so significant tension and its resulting decrease in blood supply can make an incision heal poorly. The amount of tension that is appropriate is nearly infinitely variable based on the person, the surgery, the part of the body where the incision is located, and a whole host of other factors. This is why there is no simple formula to determine ideal tension and why surgeon experience is so critical. Too much tension and the scar heals poorly. Too little tension and the result will not be as good as it could be.
Inflammation: Inflammation sounds like a bad thing but it is actually a necessary part of good healing. Too much inflammation is bad and it can result in more scar tissue both at the skin level and internally. The body uses inflammation to heal. It sends specific cells into the area of injury, like the surgery area, to clean up whatever tissue needs to be cleaned up and get the collagen building phase of wound healing started. The four main steps of healing are Hemostasis, Inflammation, Proliferation, and Remodeling. Each stage is important so spending too much or too little time in any stage can result in some form of less than ideal scar/healing. The things that can prolong the inflammatory phase are many but the main ones are: contamination/infection, suture inflammation, excessive tissue injury. These can and should be controlled as much as possible by the surgeon. Gentle tissue handling is important, so is maintaining a clean and sterile operating room environment. The use of low-inflammatory sutures, their placement, and how the wound is closed and supported are also important in reducing the length of time in the inflammatory phase of wound healing.
Location/orientation of incision: Our skin has—by virtue of gravity, how we move, and how it develops—natural creases and folds. These are the ideal areas where incisions should finally rest after surgery. Incision that are perpendicular to these natural folds or otherwise work against the natural way that body would like to have things are at increased odds of healing with some form irregularity that can detract from the final scar appearance. Much of the process of placing the final incision in the ideal area is visualization, by the surgeon, of how the skin will move during surgery and after surgery and designing the surgery to work with the body, with gravity, and with natural movement.
So, let’s look at some examples.
There is the general consensus that darker skin individuals can have thicker scars such as hypertrophic scars or keloid scars especially with body contouring procedures. As discussed above, we cannot control genetics, but we can try and control everything else to minimize the role of genetics. The photo below shows that when all goes well, a darker skin individual can get a tight tummy tuck result with a good incision scar appearance.
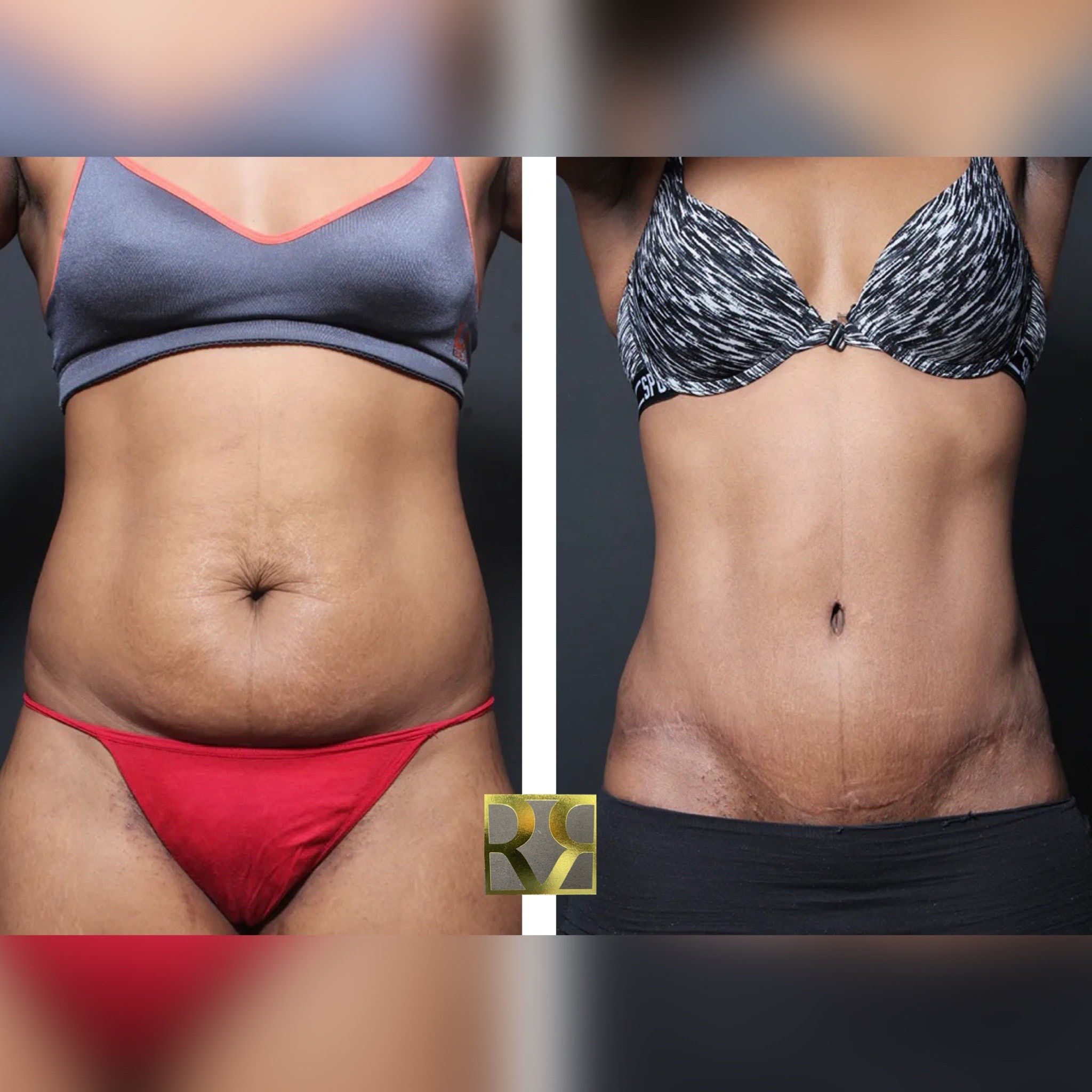
We can imagine a scenario for the patient above where any more tension added to the incision would have resulted in a thick hypertrophic scar detracting from the overall final result. Conversely, we can also imagine taking less skin during the tummy tuck, reducing tension to achieve the same type of incision appearance, but not getting as good of a contouring result. For ideal results, the ideal amount of tension is sometimes a fine balance, threading a narrow path between too much and too little tension.
The patient shown below is a recent patient that is about 3 months out after a tummy tuck. I have added the photo here because the ideal incision location has to take into account not only where the loose skin is before surgery, but also what the final ideal contour will be after surgery. By doing so not only is the incision location ideal for clothing and overall appearance but it also blends better with the structures of the body after surgery—hips and waist.
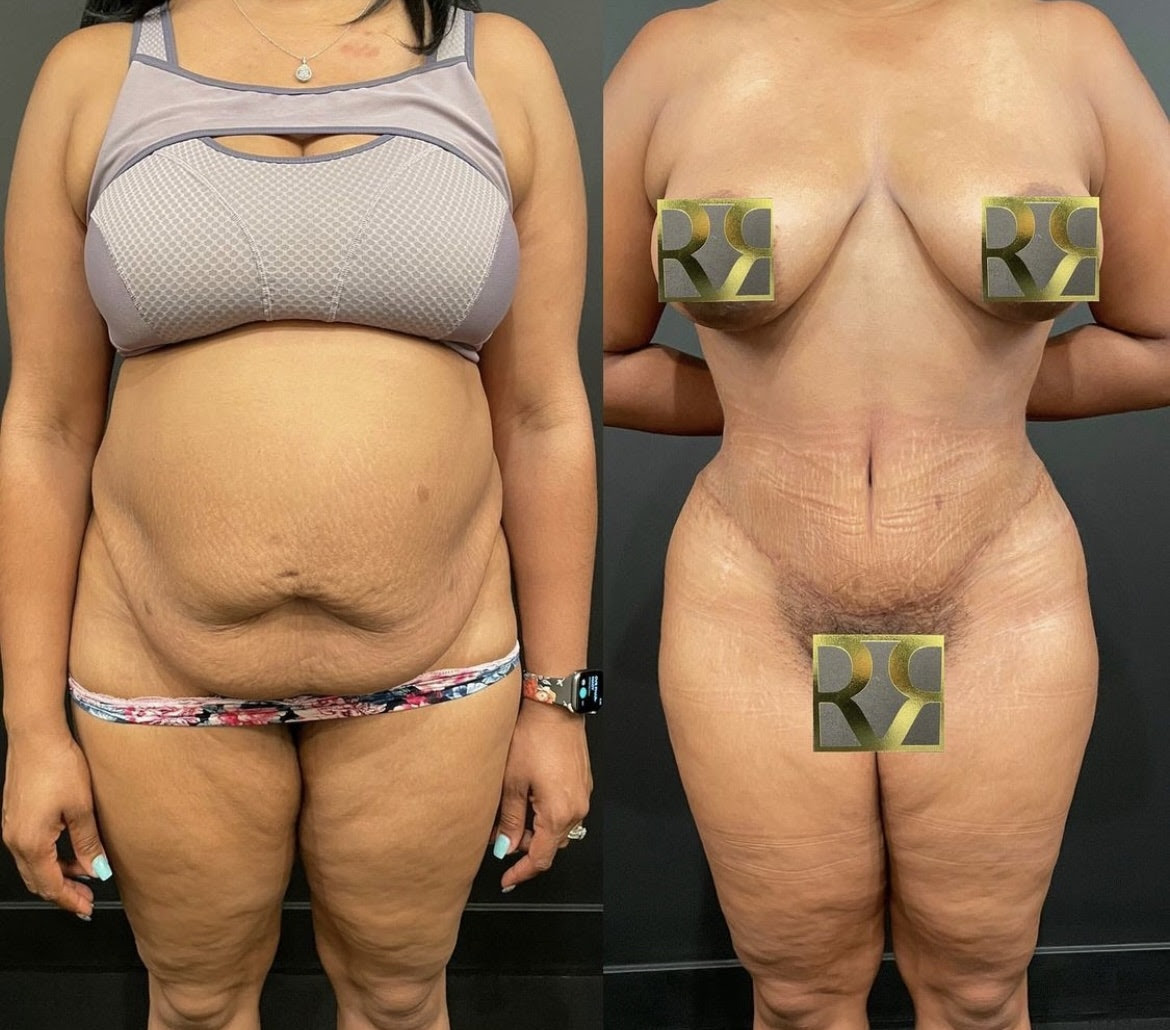
Scarring remains an important concern for anyone having surgery. By working with nature (anatomy, physics, physiology) and by envisioning how the body will be after surgery, the best combination of tension, location, and technique can be used to make the incision as inconspicuous as possible.
Remus Repta, MD

