If you are a plus size patient seeking a tummy tuck chances are you have been turned down and told that it is not safe to do so. Regardless of how much back pain, mobility restriction, skin chaffing, and other issues the excess skin and fat may be causing you the most common surgeon response is that you must lose weight first.
Over the last fifteen years, I have worked to better understand and modify plus size surgery. This work culminated in the Plus Size Tummy Tuck® which I designed to take into account all of the health parameters of the patient (more about this below) and allow the plus size patient to safely and effectively benefit from removal of excess tissue and waist contouring.
Let’s start by defining “plus size” and “safe” and then I will discuss why we may have missed and are still missing the opportunity to help plus size patients. Have a look at one of our patients shown below. It’s easy to see how this patient and patients like her, would be tremendously helped in terms of mobility, physical health, and mental health after a Plus Size Tummy Tuck®.
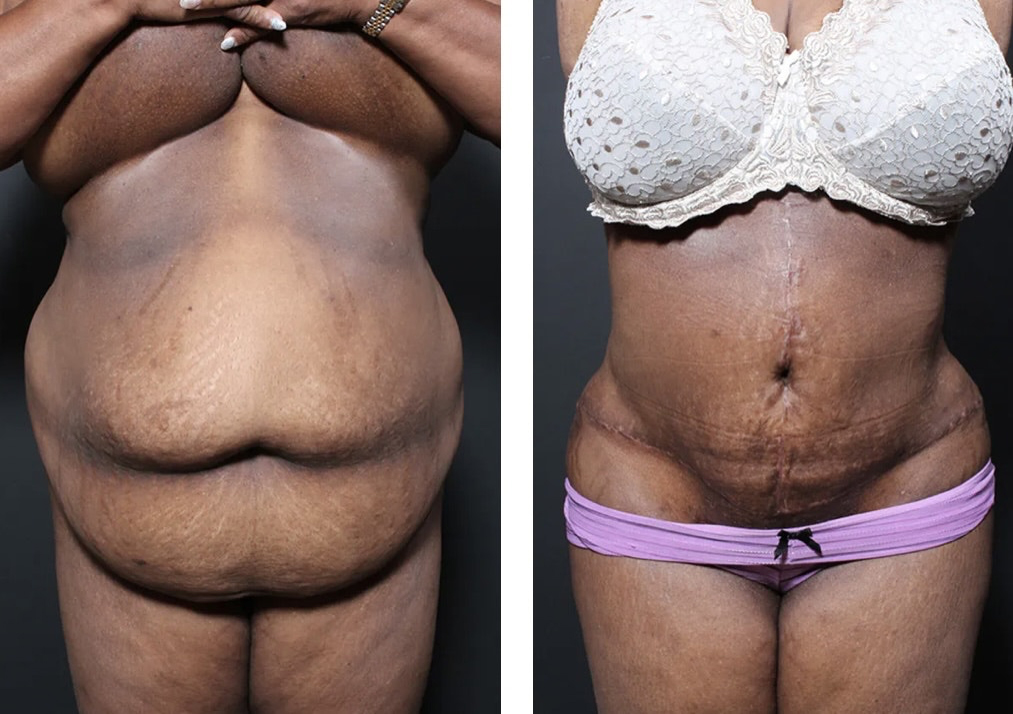
So, what defines who is plus size? The simple answer is body mass index (BMI). The BMI is defined by your height and weight—that’s it! As you can already tell from the simplicity of that calculation that’s not a lot of information. You can be healthy or sick, very little muscle mass or a body builder—the BMI does not make any distinction—and we have been using this seemingly arbitrary measurement to essentially decide who can have surgery and who should not. The BMI does not take into consideration any other patient health data. Heart, lungs, diabetes, medications, prior surgery—none of these nor any other health data is taken into account for calculating BMI. Perhaps equally important, there is no consideration of how the surgery can or should be done. After all, not all tummy tucks are created equal. A poorly designed, poorly performed tummy tuck will result in complications in the healthiest patient with the most “ideal” BMI.
So how did the BMI become the benchmark for body contouring safety?
During the 80’s, as the overall weight of the western population began to increase, anecdotal and peer reviewed scientific evidence began to point to a correlation that larger patients, patients with a higher BMI, tended to have higher complication rates when they underwent certain body contouring procedures such as abdominoplasty (aka tummy tuck). So it would make some sense then, that the response to a patient with a higher BMI requesting a tummy tuck should be to turn down the patient until they have reduced their weight to some appropriate level. The data as to what BMI is “appropriate” is, as is frequently the case, not particularly specific. The plastic surgery community, has tended to focus on a BMI of around 30-35, below which, surgery would be “safe” and above which surgery would be “unsafe”.
Despite the limitation of using just the BMI to determine who can have surgery and who should not, the correlation became the guiding principle and plus size patients, patients who were overweight while otherwise healthy, were deemed unsafe for body contouring surgery such as tummy tucks.
I completed my plastic surgery residency training in June 2008. As part of that training and in order to become board certified by the American Board of Plastic Surgery (ABPS) each surgeon must pass a rigorous written and in person examination. Everything about those two gateways to being board certified focus on the surgeon’s decision making ability related to safety and ethics. Technical skills are also evaluated indirectly by the each surgeons complication rate, but evaluation of the decision making process is more of a focus and certainly easier to decide, in a binary fashion, whether a candidate is “safe”.
Why is this important? First do no harm! This is the mainstay of the Hippocratic Oath which all doctors must abide by. In large part because of that, much of the focus in plastic surgery training and in the board certification process centers on safety—and you can’t be safe if you make bad decisions.
Unfortunately, I think we have been asking ourselves the wrong question. Instead of “At what BMI should patients be allowed to have a tummy tuck?” we should be asking “How can I modify the tummy tuck process from beginning to end, from patient selection to patient education, to tummy tuck design, to post-operative management, so the plus size patient can have a safe and effective tummy tuck/surgery?” This is essentially the question I have been asking myself the last fifteen years and the result of that answer has been the safety and efficacy of the Plus Size Tummy Tuck ®. After all, plus size patients do benefit both physically and mentally from removing 10, 20, sometime 30 pounds of tissue that is hanging off of their abdomen and onto their lap.
The magical part of plastic surgery and one of the reasons I became a plastic surgeon, is that you have a chance to help patients. Not only that, but you are able to do so with your hands and with the ingenuity of your own mind and the minds of the surgeons before you. When faced with a challenge the plastic surgeon doesn’t say it can’t be done—the plastic surgeon says how can I figure out a way to solve this challenge.
It’s been fifteen years since I started this journey of helping plus size patients. We have learned a lot and we are learning a little more each time we do a Plus Size Tummy Tuck ®. I am grateful and excited to see where the next fifteen years will take us.

